
MEN: Porn, Shame, and Mental Health: How to Break the Guilt Cycle Without Self‑Sabotage
Quick Answer
Name the shame loop, install blockers across devices, use a brief self-compassion script after slips, and run a weekly review. Anchor sleep and exercise to steady mood, since adults do best with 7 or more hours of sleep and 150 minutes of weekly activity with 2 strength sessions [10][11].
This is education, not medical advice.
Jump to: Quick Comparison | The Simple Framework | FAQ
Disclosure: MenTools publishes this article and may feature MenTools products.
How we evaluate: Products are assessed on nutrient form quality, dose vs NRV, authorised health claims, male-specific design, and independent research. Full sources are listed in the references below.
Quick Comparison
| Approach | Tackles | Time | Cost | Best For |
|---|---|---|---|---|
| Self-compassion break | Self-attack | 1–3 min | Free | Shame spikes [8][9] |
| CBT reframing | Catastrophising | 2–6 wks | Free | Rumination [12] |
| Blockers + accountability | Access, secrecy | Now | Free | High-risk devices [1][6] |
| Trigger mapping | Cue awareness | 1–2 wks | Free | Patterns [6] |
| Mindfulness urges | Urge surfing | 5–10 min | Free | High arousal [3] |
| Sleep and exercise | Stress load | 2–4 wks | Free | Mood, energy [10][11] |
| Support group or therapy | Isolation | 4–12 wks | Varies | Comorbidity [7] |
| Emergency reset plan | Relapse control | Now | Free | Slips [2] |
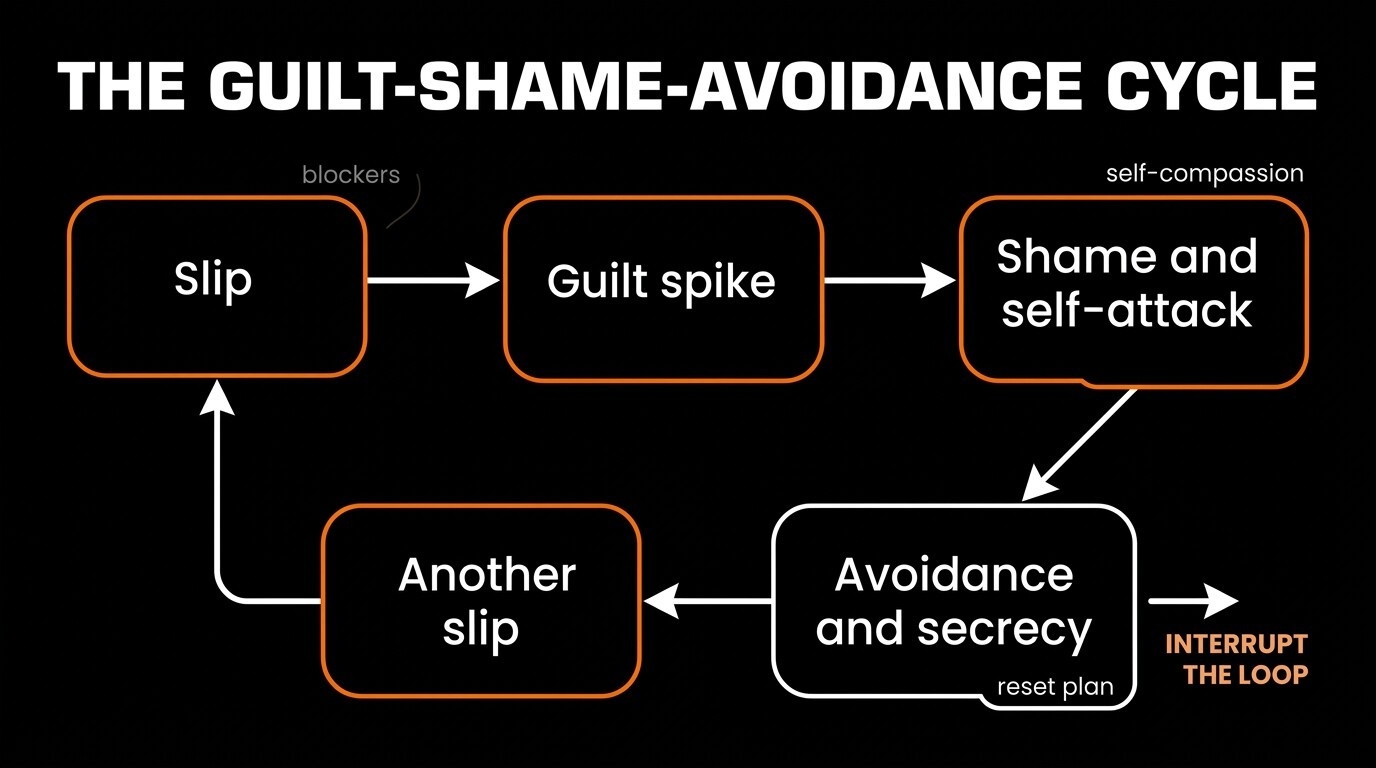
The guilt-shame-avoidance cycle: how each stage feeds the next and where practical tools interrupt it.
The Real Answer
What is the guilt-shame-avoidance cycle?
After a slip, many men hit the abstinence violation effect: “I blew it, so the streak is ruined,” which increases avoidance and risk of bingeing [2]. Naming the loop reduces reactivity and opens space to run your reset plan instead of hiding.
Shame thrives in secrecy and unstructured time. With 85 per cent of adults carrying smartphones, access is constant unless you add friction on the highest-risk device [1].
How does self-criticism increase relapse risk?
Harsh self-talk raises shame and avoidance, both associated with worse outcomes in behavior change domains [8]. A brief self-compassion pause shifts attention from punishment to the next effective step without excusing behavior [9].
Treat slips as data. The question moves from “what is wrong with me” to “what cue did I miss and which plan do I run now” [2].
When should you screen for anxiety or depression?
Screen if use escalates alongside persistent low mood, anhedonia, restlessness, or sleep problems. Scores of 10 or higher on the PHQ-9 and GAD-7 indicate at least moderate symptom levels that merit a clinician conversation [4][5].
Early identification reduces guesswork and improves care pathways. Pair screening with device controls to lower immediate risk while you seek support [1].
Do blockers and accountability reduce shame spirals?
Yes. Stimulus control and environment redesign reduce cue-triggered responding by increasing friction at the moment of decision [6]. Gentle accountability or peer support counters isolation and can improve adherence in recovery settings [7].
Practically, this means securing the phone first and agreeing to simple weekly check-ins. Less secrecy means fewer opportunities for the shame loop to escalate [1].
Does self-compassion improve behavior change?
Self-compassion is linked with less self-criticism and better follow-through on health behaviors after setbacks [8]. It works as a reset button that restores perspective and values so you can act on your plan [9].
Keep it short. Ninety seconds or less is often enough to interrupt the spiral and pivot to your if-then action [8].
Why This Fails
- All-or-nothing streaks, hidden devices, and rumination without plans.
- Treating shame as motivation instead of a risk factor.
- No sleep or movement anchors to stabilise mood.
How to Fix It
The Simple Framework
- Name: say “shame-avoid-slip” aloud or in a note when it starts.
- Normalise: slips are data, not destiny.
- Plan: blockers on phone and if-then scripts in high-risk windows.
- Practice: rehearse self-compassion and the reset plan when calm.
- Review: 5 minutes weekly to tweak one blocker and one script.
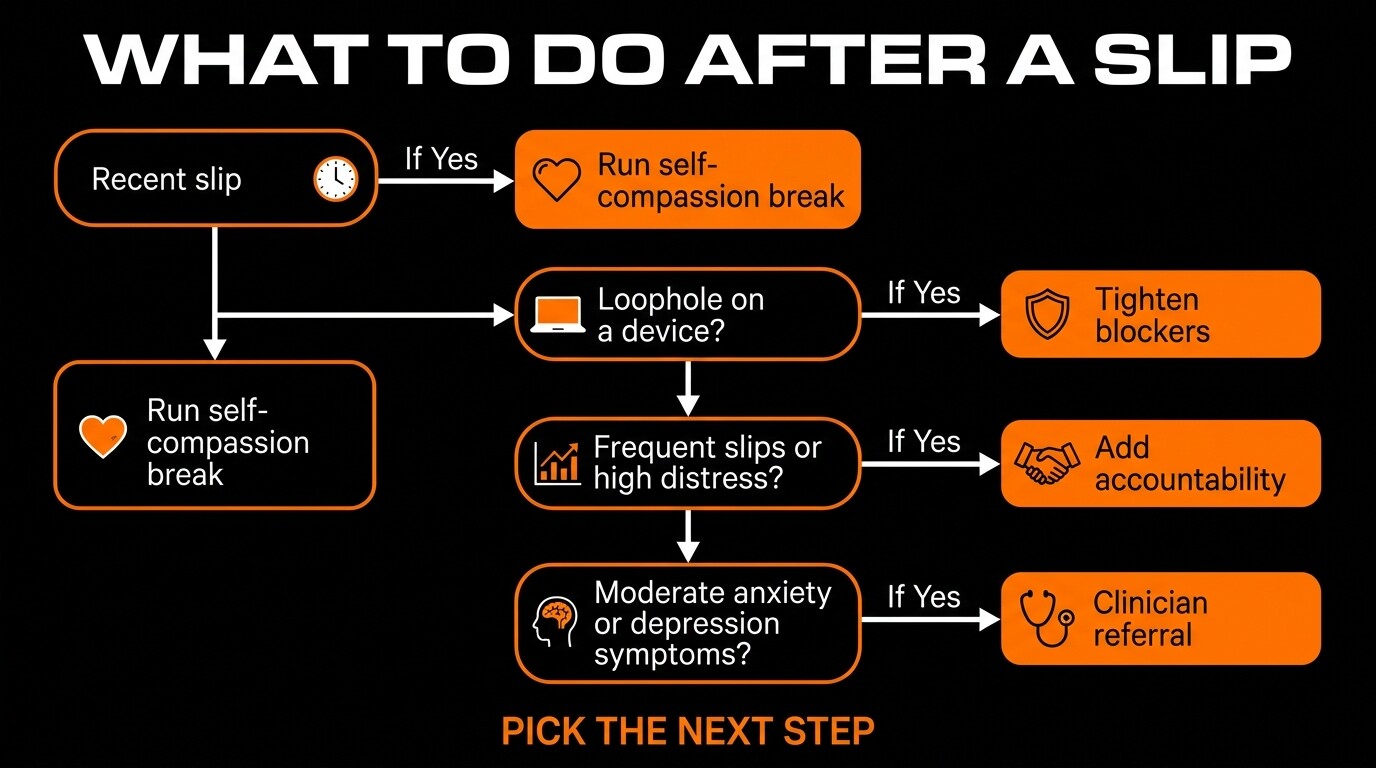
Which tool fits your situation: a decision flowchart for men choosing between self-help approaches and professional support.
5-step plan
- Write two rules and your why. Pick two clear rules, for example: no explicit content on phone and no private browsing after 10 pm. A one-sentence why clarifies values when urges spike [2].
- Install blockers and tell one person. Secure phone, laptop, and wifi, since mobile access is the primary loophole for most men [1]. Share your rules with one trusted person to reduce secrecy and increase follow-through [7].
- Map triggers and if-then plans. List top three cues by time, place, and state. Implementation scripts paired with environmental friction reduce automatic responding to cues [6].
- Use a self-compassion break after slips. Sixty to ninety seconds: notice the feeling, name the loop, normalise being human, and choose the next best action [8][9]. Follow with a 10-minute replacement activity or a walk to downshift arousal [3].
- Sleep 7+ hours and add two workouts. Adults benefit from 7 or more hours of sleep nightly and about 150 minutes of weekly moderate activity with 2 strength sessions for mood and stress regulation [10][11]. New habits typically take weeks to feel automatic, with a median of about 66 days across behaviors, so be patient and consistent [12].
FAQ
Is guilt helpful or harmful for change?
Guilt can prompt repair, but shame and self-attack tend to drive secrecy and relapse via the abstinence violation effect [2]. Use guilt as feedback and pivot to concrete next actions.
How do I stop shame after a slip?
Run a 60-second self-compassion script, then execute your emergency reset: leave the room, open your plan, and start a 10-minute alternative task or walk [3][8]. Follow up by tightening blockers in the exact loophole used [6].
What if partners or faith add pressure?
Align with your values while keeping changes doable. Share your rules and weekly review plan rather than obsessing over streaks, which fuels the shame loop [2].
When do I need a therapist or doctor?
If your depression or anxiety screeners reach moderate levels, or you have safety concerns, involve a clinician for assessment and care [4][5]. Professional support pairs well with device controls and habit planning.
Can mindfulness replace blockers?
No. Mindfulness helps you ride urges, but stimulus control reduces exposure at the source, and the combination is stronger than either alone [3][6].
How long until shame eases?
Many men feel relief within 2 to 4 weeks as blockers reduce exposure and routines stabilise, especially with better sleep and regular movement [10][11]. Full habit automaticity often takes longer, with a median of about 66 days [12].
Final Recommendation
Pair device controls with a short self-compassion protocol and weekly reviews. Protect sleep and movement to lower stress load, and keep plans visible and simple so you can execute under pressure [1][8][10][11].
Options For Men to Take Action
The fastest and most cost-effective way for men to take action is through the MenTools Quit Porn Protocol. This all-in-one system helps you install blockers, write if-then scripts, add accountability, access tons of tools and run a structured reset, all from the convenience of your phone.
Last updated: 2026-03-04 v1.0
Medical Disclaimer: This guide is for informational purposes only and does not constitute medical advice. Always speak with your doctor or another qualified healthcare professional before starting any new supplement or programme if you have medical conditions or take prescription medication.
References
- Pew Research Center. Mobile Fact Sheet. https://www.pewresearch.org/internet/fact-sheet/mobile/
- Hendershot CS, Witkiewitz K, George WH, Marlatt GA. Relapse prevention for addictive behavior. Addiction. 2011. https://pubmed.ncbi.nlm.nih.gov/21491319/
- Bowen S, Chawla N, Collins SE, et al. Mindfulness-based relapse prevention randomized trial. JAMA Psychiatry. 2014. https://pubmed.ncbi.nlm.nih.gov/24690908/
- Kroenke K, Spitzer RL, Williams JB. The PHQ-9 validity study. Journal of General Internal Medicine. 2001. https://pubmed.ncbi.nlm.nih.gov/11556941/
- Spitzer RL, Kroenke K, Williams JBW, Löwe B. The GAD-7 validation. Archives of Internal Medicine. 2006. https://pubmed.ncbi.nlm.nih.gov/16717171/
- Wood W, Neal DT. A new look at habits and the habit-goal interface. Psychological Review. 2007. https://pubmed.ncbi.nlm.nih.gov/17500626/
- Kelly JF, Humphreys K, Ferri M. Twelve-step programs for alcohol use disorder, Cochrane review. 2020. https://pubmed.ncbi.nlm.nih.gov/32074412/
- Sirois FM, Kitner R, Hirsch JK. Self-compassion and health behaviors. Health Psychology. 2015. https://pubmed.ncbi.nlm.nih.gov/25133852/
- Neff KD. Self-compassion: An alternative conceptualization of a healthy attitude toward oneself. Self and Identity. 2003. https://self-compassion.org/wp-content/uploads/publications/SCinSelfIdentity.pdf
- Centers for Disease Control and Prevention. How much sleep do I need. https://www.cdc.gov/sleep/about_sleep/how_much_sleep.html
- Centers for Disease Control and Prevention. Adult physical activity guidelines. https://www.cdc.gov/physicalactivity/basics/adults/index.htm
- Lally P, van Jaarsveld CH, Potts HW, Wardle J. Habit formation in the real world. European Journal of Social Psychology. 2009. https://onlinelibrary.wiley.com/doi/10.1002/ejsp.674


